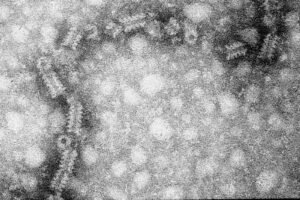
Mumps Disease
| General Studies Paper II: Disease, Government Policies |
Why in News?
Recently, mumps cases in the United States have seen a notable rise in early 2026, with 34 cases reported across 11 jurisdictions by late February. Despite high vaccination rates, cases persist in vaccinated young adults, largely due to waning immunity years.
What is Mumps Disease?
- About: Mumps is a viral infectious disease characterized primarily by painful swelling of the salivary glands, especially the parotid glands located near the ears.
- According to the World Health Organization, it is a vaccine-preventable disease that mainly affects children and adolescents but can occur at any age.
- Causative Agent: Mumps is caused by the Mumps virus, a single-stranded RNA virus belonging to the Paramyxoviridae family and Rubulavirus genus.
- Incubation Period: The incubation period typically ranges from 16–18 days, though it may vary between 12 and 25 days. During this phase, the infected individual usually shows no symptoms but can still transmit the virus to others.
- Transmission: Mumps spreads mainly through respiratory droplets, saliva, and direct contact with infected secretions. Activities such as coughing, sneezing, sharing utensils, or close physical contact significantly increase the risk of virus transmission.
- Major Symptoms: The most recognizable symptom is parotitis, or swelling of the parotid salivary glands, causing puffy cheeks and jaw pain.
- Other symptoms include fever, headache, muscle aches, fatigue, and loss of appetite.
- Affected Population Groups: Mumps mainly affects unvaccinated children aged 5–14 years, but outbreaks can also occur among young adults, particularly in schools, colleges, hostels, and military barracks where close contact facilitates viral spread.
- Complications: Though often mild, mumps can cause serious complications such as orchitis (testicular inflammation) in males, oophoritis in females, meningitis, encephalitis, and permanent hearing loss in rare cases.
- Diagnosis Methods: Diagnosis is usually based on clinical symptoms, especially parotid swelling. Laboratory confirmation may involve RT-PCR testing, serological tests detecting IgM antibodies, or viral isolation from saliva or throat swabs.
- Treatment: There is no specific antiviral treatment for mumps. Management focuses on symptomatic relief, including rest, hydration, pain relievers, and cold compresses to reduce gland swelling and discomfort.
- Vaccination: The most effective preventive measure is the MMR vaccine (Measles–Mumps–Rubella). Two doses of the vaccine provide about 88% protection against mumps.
- Immunity: A person who recovers from mumps generally develops long-term immunity against the virus. However, partial immunity may occur in rare cases.
Global and Indian Burden of Mumps Disease
- Global Scenario:
-
- Case Burden: According to the World Health Organization, about 500,000 cases of mumps are reported globally each year, although the true burden may be higher because the disease is not notifiable in many countries. In 2023, around 384,785 cases were officially reported worldwide.
- Distribution: The epidemiology of mumps varies across WHO regions. Higher incidence has been observed in low- and middle-income countries due to gaps in vaccination coverage. For example, the African region reported an incidence as high as 761 cases per million population in 2023, while other regions show relatively lower.
- Immunization Status: By 2024, about 124 countries had introduced mumps vaccination as part of national immunization schedules. However, uneven vaccine coverage and immunity gaps still allow outbreaks to occur in several regions.
- Resurgence: Despite high coverage with the MMR (Measles-Mumps-Rubella) vaccine, outbreaks have been reported in countries such as United Kingdom, Canada, Spain, and Netherlands. These resurgences are linked to waning immunity and close-contact environments like universities.
- Economic Impact: Mumps outbreaks create a significant economic burden due to healthcare costs and productivity loss. Studies estimate that each mumps case in developed countries may cost around US$9,459. A study from the United States estimated an average cost of about $9,459 per case.
- India:
- Case Statistics: India continues to report tens of thousands of mumps cases annually. Government data for 2023–24 recorded about 62,406 cases and five deaths across the country, indicating that the disease remains endemic in several regions.
- Distribution: The burden varies widely between states. Kerala reported the highest number of cases (over 30,000) during 2023–24, followed by states such as Maharashtra, Karnataka, Gujarat, and Assam, showing strong regional clustering of outbreaks.
- Outbreak Patterns: India frequently experiences localized outbreaks, particularly in schools and densely populated areas. For example, Kerala recorded over 11,000 cases within two months in 2024, while smaller clusters have also been documented in other states.
- Surveillance: Unlike some infectious diseases, mumps is not a separately notifiable disease in the Integrated Disease Surveillance Programme (IDSP). Cases are often reported under the “other diseases” category, which may lead to underreporting and incomplete epidemiological data.
- Concerns: Major concerns include low vaccination coverage for mumps, population density, and delayed detection of outbreaks. Many children remain unvaccinated or partially vaccinated, which allows the virus to circulate and cause repeated outbreaks in communities.
International Guidelines and Global Initiatives to Control Mumps
- WHO: The World Health Organization (WHO) provides global guidance for controlling mumps, emphasizing immunization, surveillance, and outbreak response.
- Under the World Health Organization’s Immunization Agenda 2030, countries are encouraged to strengthen routine immunization systems and ensure equitable access to mumps-containing vaccines worldwide.
- The WHO recommends mumps vaccination only if a nation can sustain 80% coverage to prevent infections in older adults.
- Two-Dose Schedule: Global guidelines mandate a two-dose protocol. Children receive the first dose at 12–15 months and the second at 4–6 years. This system reduces vaccine failure and ensures the strongest possible community immunity against the virus.
- The CDC now recommends a third MMR dose during intense outbreaks. It addresses waning immunity that occurs years after the initial childhood series is completed.
- Molecular Surveillance Systems: Health agencies use the Global Measles and Rubella Laboratory Network. They track specific virus genotypes using RT-PCR tests. This helps scientists determine if an outbreak started locally or arrived from another country.
- Five-Day Isolation Rule: International protocols require patients to isolate for five days. This period starts when the parotid glands begin to swell. Rapid isolation stops the spread of respiratory droplets in schools and crowded workplaces.
- Healthcare Worker Immunity: Guidelines require all medical staff to show documented immunity. Doctors and nurses must have two vaccine doses or a positive antibody titer test. This prevents the virus from spreading to vulnerable patients in hospitals.
- Cold Chain Management: Initiatives focus on strict vaccine storage temperatures. The vaccine must stay between 2°C and 8°C. If the “cold chain” breaks, the vaccine loses its potency, leading to outbreaks even in vaccinated groups.
- Public Awareness Campaigns: Global initiatives include risk communication for parents. They educate families about rare complications like meningitis and permanent deafness. Organizations such as UNICEF and Gavi, the Vaccine Alliance support global mumps control by educating people.
India’s Strategy to Control Mumps
|
| Also Read: FDA Approves First Therapy for Menkes Disease |